- Home
- Patient Area
- Early Onset Scoliosis
What is early onset scoliosis?
Early onset scoliosis is a scoliosis that develops before the age of 10 years of age. It has also been called infantile scoliosis and juvenile scoliosis.
The cause for early onset scoliosis can be unknown (idiopathic) or due to a number of other causes that result in a scoliosis under the age of 10 years. Some of those causes are described here.
Early onset scoliosis has been abbreviated to EOS.
A scoliosis means that the spine is curved abnormally when viewed from the front or the back. It can lead to the trunk and shoulders no longer being symmetrical. Sometimes the shoulders aren’t level anymore. Sometimes the head is not level or the pelvis is not level. The rib cage can also push out on one side so that it becomes prominent - this is known as a rib hump. The severity of the abnormalities can vary between people and can change with time.
How would I know my child had early onset scoliosis?
Either you, your child or someone else may notice that you or your child is not standing straight or that they have changes in the shape of their spine.
You may notice:
- Rib cage sticking out on one side especially at the back
- Shoulders not being level
- The hip or waist sticking out
- The head tilting over to one side of the trunk
- Clothes not fitting well anymore
- Not being able to stand up straight
- There may be pain as well as the changes above (rare)
Why does it matter?
Sometimes the shape changes can make your child feel very awkward as they get older. Some people do get very embarrassed about their shape. The shape can change as your child grows, particularly at the time of growth spurts.
If scoliosis worsens, it can affect the mechanics of your spine and result in aching or pain.
Occasionally, especially if the scoliosis affects someone early in life, it can affect the development and function of the lungs. This does need to be treated or at least monitored. The younger the age when the scoliosis starts, the more likely this may happen. If not monitored and treated when appropriate, this type of scoliosis can result in serious health problems related to the lungs in adulthood. These problems can be bad enough to affect daily life and ultimately affect the heart.
Generally, a scoliosis that has started early in life, can get a lot bigger due to all the growth that the spine will go through. A bigger curve can cause more of the problems described above.
What should I do if I think there is an early onset scoliosis?
Speak to your GP. Your GP will be able to assess and see if there is a scoliosis.
If your GP is concerned, they will refer you to a Spine Surgeon, Paediatrician or Orthopaedic Surgeon at a hospital for further tests.
Once a scoliosis is confirmed, you will need to see a Spine Surgeon at a recognised spine centre who will assess you fully and talk about what you may need. The GP, Paediatrician or Orthopaedic Surgeon will refer you on to the Spine Surgeon.
Do not ignore it if you think there is an early onset scoliosis. Remember, if proven, this is the type of scoliosis that needs careful monitoring.
How will the doctors check for a scoliosis?
 The first thing the specialist will do is talk to you about your concerns. They will ask questions about health generally, how the problems are affecting your child and try to get an idea how much more growth and development there is left.
The first thing the specialist will do is talk to you about your concerns. They will ask questions about health generally, how the problems are affecting your child and try to get an idea how much more growth and development there is left.
The doctors will want to examine the spine and so your child will need to be undressed for this. Often the hospital will give you a gown, but wearing shorts and a T shirt may make things easier. The examination will look at the back and see how flexible it is. They will often look at the back whilst bent forwards as this reveals the scoliosis more (Adam’s position). Your child’s arms and or legs will often be examined to make sure the spinal cord is working normally.
The Spine Surgeon will send your child for X - rays. These are necessary to see if there is a scoliosis and how bad it is. The Spine Surgeon will measure the angle of the scoliosis on the X - ray (Cobb angle). The X - rays also show if there are causes for the scoliosis. Sometimes the X - rays help to identify if there is a high risk of the scoliosis worsening.
After all of this, the doctors may want you to go for further tests such as an MRI scan. If your child is very young, an MRI scan may need a general anaesthetic to help them stay still in the scanner. The doctors will talk that through with you. If the plan is to monitor your scoliosis, you will be asked to return in a few months (often 6 months) for another examination and X - ray.
How can you treat early onset scoliosis?
Observation
The commonest initial plan is to be monitored. This will be by 6 - 9 monthly appointments at the hospital by the Spine Surgeon. The appointment will usually involve being examined again and having an X - ray. This is to see if the scoliosis is worsening. If it remains roughly the same each time you are seen then they will continue to monitor you until you are fully grown.
Exercise
There is no need to avoid sport or exercise when you have EOS. It is actually better for you to remain active and to have good core muscles. Unfortunately there is no strong evidence that exercise alone stops a scoliosis progressing or improves it. There are many ongoing studies that may help prove the role of exercise one way or another.
Casting or Bracing
In very young children and babies, the initial treatment is often a plaster jacket. This is usually applied under general anaesthetic and changed 3 monthly. It can take some time for you to get used to your child having a non removable plaster jacket and practical issues such as using a nappy over the jacket. You will get support for all of this. Plaster jackets are a well established method of controlling a child with EOS.
Sometimes a removable brace is suggested once your child is old enough for this to be fitted. The braces are usually rigid and need to be worn 23 hours a day. They can be worn under your child’s clothes. It has been found that braces only work if they are used more or less constantly. You can take the brace off to wash, dress and during sporting activities.
Surgery
Surgery may be necessary if the curve in the spine is worsening or is very bad to begin with.
Surgery in a growing child’s spine aims to reduce the risk of the curve worsening at the same time as trying to ensure the spine overall still grows and lengthens with time.
To achieve these aims, rods have to be used along with implants to connect the rods to the bones of the spine (hooks, screws or wires).
It is inevitable that more than one operation may be needed. The main reason for this is that we are trying to avoid stunting the growth of the spine, so repeat operations are needed to stretch the spine or to change the length of the rods. As the spine bones are often small when an operation is first needed, the hooks or screws used to control the spine may loosen and need replacing. The ongoing growth of the rest of the spine can also lead to new curves developing that need treatment. Once it is felt that the amount of growth left in the spine is minimal, a final operation to fuse the spine may be planned. This is to help control the scoliosis for good.
The commonest operations for EOS are as follows:
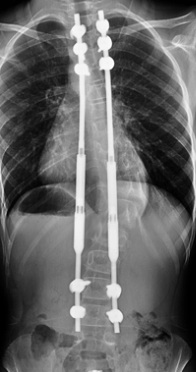
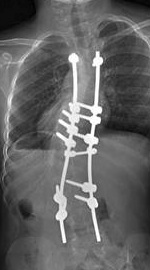
Surgically lengthened growing rods - this involves rods that are stretched out every 6-9 months by a small (often daycase) procedure to try to maintain spine length.
Magnetically driven growing rods - this involves rods that are stretched out at regular intervals by using a remote control on a magnet on the rods. The magnet mechanism lengthens the rods. This can be done in a clinic and does not need a repeat operation for the lengthening. Operations may be needed if a longer rod is needed or the magnet stops working. The MAGEC rod is an example of this.
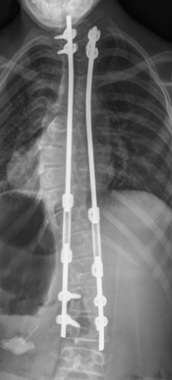
Growth guidance systems - this involves rods connected loosely to screws on the spine. The idea is that the rods control the spine, but as they are loosely connected the spine can slide on the rod as it grows. This type of system would need fewer operations as no lengthening is required. Operations may be needed if a longer rod is needed. The Shilla technique is an example of this.
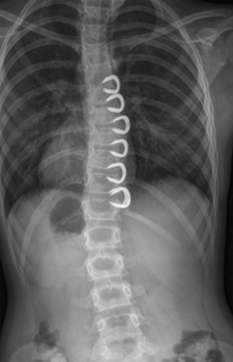
Compression based systems - this is rarely performed in the UK. This often involves surgery on the front of the spine (through an incision on the side of the chest) to put on metal implants known as staples that squeeze the growing bones. Squeezing the bones changes the way they grow to try to improve a scoliosis with time.
%20-%20JPG.jpg)